Lymphoma is a type of cancer that affects your blood cells called lymphocytes. Lymphocytes are a type of white blood cell that support our immune system by fighting infection and disease. They mostly live in our lymphatic system with only very few found our blood.
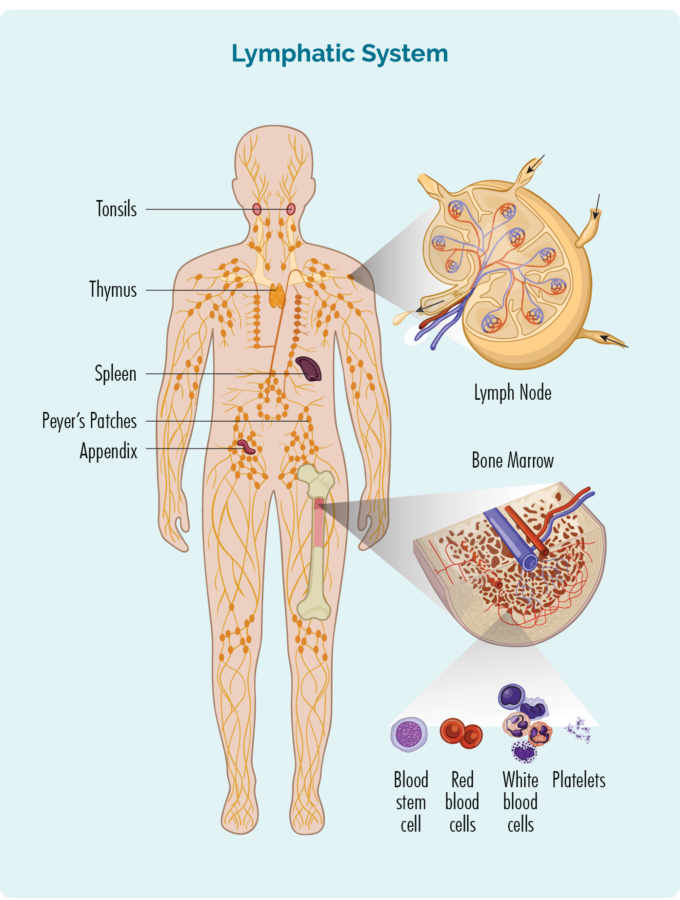
Our lymphatic system is responsible for cleaning our blood of toxins and waste products and includes our lymph nodes, spleen, thymus, tonsils, appendix and a fluid called lymph. It is also where our disease fighting antibodies are made.
Lymphoma includes 4 subtypes of Hodgkin Lymphoma, more than 75 subtypes of Non-Hodgkin Lymphoma and Chronic Lymphocytic Leukemia (CLL), with CLL being considered the same disease as Small Lymphocytic Lymphoma.

To diagnose lymphoma you will need a biopsy. A biopsy is a procedure to remove part, or all of an affected lymph node and/ or a bone marrow sample. The biopsy is then checked by scientists in a laboratory to see if there are changes that help the doctor diagnose lymphoma.
When you have a biopsy, you may have a local or general anaesthetic. This will depend on the type of biopsy and what part of your body it is taken from. There are different types of biopsies and you may need more than one to get the best sample.
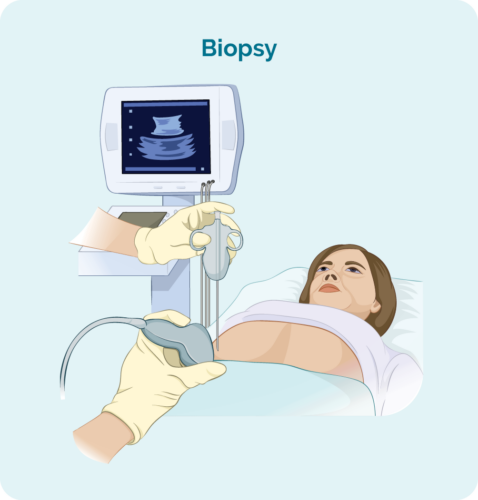
Core or fine needle biopsies are taken to remove a sample of swollen lymph node or tumour to check for signs of lymphoma.
Your doctor will usually use a local anaesthetic to numb the area so you don’t feel any pain during the procedure, but you will be awake during this biopsy. They will then put a needle into the swollen lymph node or lump and remove a sample of tissue.
If your swollen lymph node or lump is deep inside your body the biopsy may be done with the help of ultrasound or specialised x-ray (imaging) guidance.
You might have a general anaesthetic for this (which puts you to sleep for a little while). You may also have a few stitches afterwards.
Core needle biopsies take a bigger sample than a fine needle biopsy.
During this procedure, a surgeon will remove the whole lymph node or lump and send it to pathology for testing. You may have a general anaesthetic which will put you to sleep for a little while, so you stay still and feel no pain.
You will have a small wound with a few stitches, and a dressing over the top.
Stitches usually stay in for 7-10 days, but your doctor or nurse will give you instruction on how to care for the dressing, and when to return to have the stitches out.
Excisional node biopsies are more reliable than fine needle or core needle biopsies for diagnosing lymphoma.
Blood tests are taken when trying to diagnose your lymphoma, but also throughout your treatment to make sure your organs are working properly and can cope with our treatment.
Once your doctor gets the results from you blood tests and biopsies they will be able to tell you if you have lymphoma and may also be able to tell you what subtype of lymphoma you have. They will then want to do more tests to stage and grade your lymphoma.

To view this in a larger screen click on the toolbar above the book on the symbol that looks like 4 little arrows pointing to each corner of a square.
See the image with icon circled in red for which symbol to click.
Once it opens in the full screen you can move back and forth by clicking on the arrows the left and right of the pages.

If you would like to download your own copy to keep on your compuiter, or print, click on the 3 dots on the toolbar above the book. After you click on the dots click on Download PDF File.
See the image with the blue circles for which symbol to click.
Throughout the booklet you will see some words in blue and underlined. Click on those blue words to open a new window with more information on that topic.
To understand lymphoma, you need to know a bit about your B-Cell lymphocytes.
B-Cell lymphocytes:
Lymphoma develops when some of your B-cell lymphocytes (B-cells) become cancerous. They grow uncontrollably, are abnormal, and do not die when they should.
When you have lymphoma your cancerous B-cells:
Some lymphomas grow very quickly, which means the cancerous B-cells are multiplying (making new copies of themselves). Other cancerous B-cells may live longer than they should.. B-cells (and many other cells) are designed to live for a purpose. Once they have achieved that purpose, they naturally die to make room for new stronger healthy B-cells.
In some cases, lymphoma develops when the cancerous B-cells just keep living even when they have no purpose. They then take up too much room which can stop your body making new healthy cells.
Please note:
Lymphoma Australia staff are only able to reply to emails sent in English language.
You need healthy T-cells to make CAR T-cells. For this reason, CAR T-cell therapy cannot be used if you have a T-cell lymphoma – yet.
For more information on CAR T-cells and T-cell lymphoma click here.
Special Note: Although your T-cells are removed from your blood for CAR T-cell therapy, most of our T-cells live outside of our blood – in our lymph nodes, thymus, spleen and other organs.